Admission assessments play a critical role in inpatient care. They guide early treatment decisions, support risk management, and help clinicians prioritize needs from day one.
MHO’s Reflections portal requires facilities to complete admission assessments within 3 days of admission. However, even when completed within 3 days, those assessments aren’t always immediately submitted to Reflections—and that delay is what we examined.
Our analysis focused specifically on when during the patient’s stay the admission assessment became available in Reflections. Importantly, we cannot determine how the assessment may have been used by clinicians before it appeared in the portal, but we can measure whether its submission to Reflections is associated with patient improvement.
What We Analyzed
We reviewed data from 573,355 inpatient stays across 253 facilities. For each stay, we evaluated the number of days into the patient’s stay the admission assessment was entered into Reflections.
Here’s what we found across all stays:
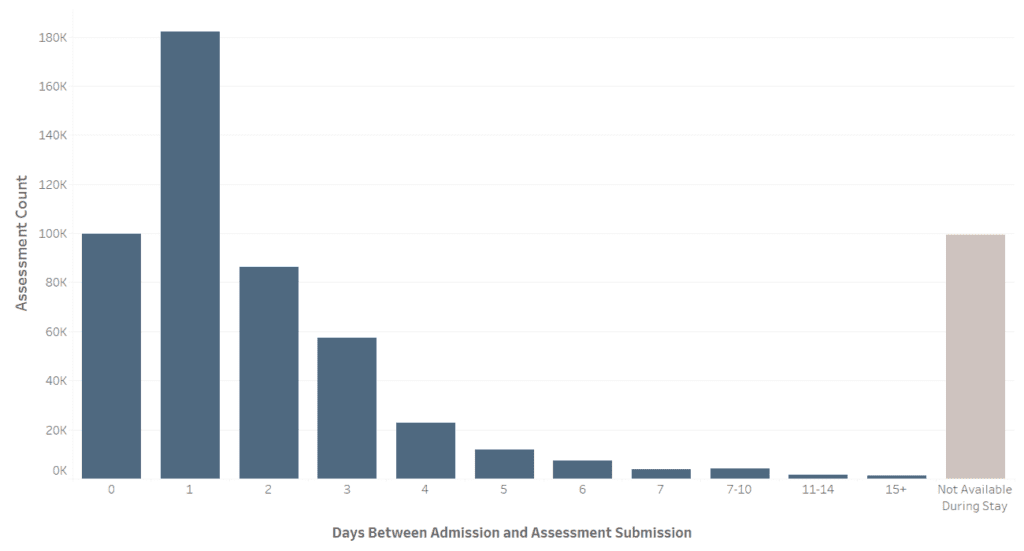
- Median delay: 2 days
Submission timing is concentrated early in the admission period, where half of all assessments are submitted at or before day 2. - Unavailable assessments: About 17% of admission assessments never became available during the patient’s stay. They did, however, appear at discharge—allowing calculation of improvement scores.
Figure 1. Delay in Admission Assessment Availability in the Patient Portal (Non–interactive visual)
To understand the impact of timing on patient improvement, we compared patients within the same facility. This removes the noise that comes from differences in staffing, patient mix, treatment models, or documentation culture across facilities.
Within a facility, are patients whose admission assessments become available later less likely to improve?
Yes. Patients experienced lower improvement rates when admission assessments were available later.
- 1‑day delay: 0.26% lower odds of improvement
- 7‑day delay: 1.79% lower odds of improvement
- Assessment not available during the stay: 5.08% lower odds of improvement
This pattern was progressive:
Longer delays were associated with lower predicted improvement.
Does This Mean Slower Facilities Have Worse Outcomes?
Surprisingly, no.
When we aggregated data, we found that facilities with longer median delays did not consistently have lower improvement rates.
Why does the relationship disappear at the facility level?
- Aggregation dilutes the effect.
A small group of patients with long delays can be overshadowed by many patients with short delays.
- Facilities treat different populations.
Some treat higher‑acuity or more complex patients. Others have faster turnover. These differences heavily influence improvement rates—sometimes more than timing does.
- Operational models vary widely.
Two facilities might have identical median delays but very different staffing models, treatment structures, or continuity-of-care practices. These broader operational factors can shape outcomes beyond documentation timing.
What’s the Takeaway?
Delays in documentation may hinder the care team’s ability to act early—but they may also reflect broader operational issues such as staffing challenges, workflow interruptions, or case mix complexity. These same disruptions could affect both documentation timing and patient outcomes.
Individual patients with no delays in admission assessment submission may thereby be more likely to improve—not necessarily because of the timing, but because timely assessment submission may be a marker of stronger operational consistency during that patient’s stay.
Recommendations
MHO’s recommended best practices emphasize:
- Reviewing admission assessments and incorporating them into treatment planning early in the stay
- Monitoring assessment submission timing patterns
- Identifying persistent or recurring delays, which often point to underlying workflow disruptions
Consistent monitoring can help facilities identify and address operational challenges that influence both documentation and patient outcomes.